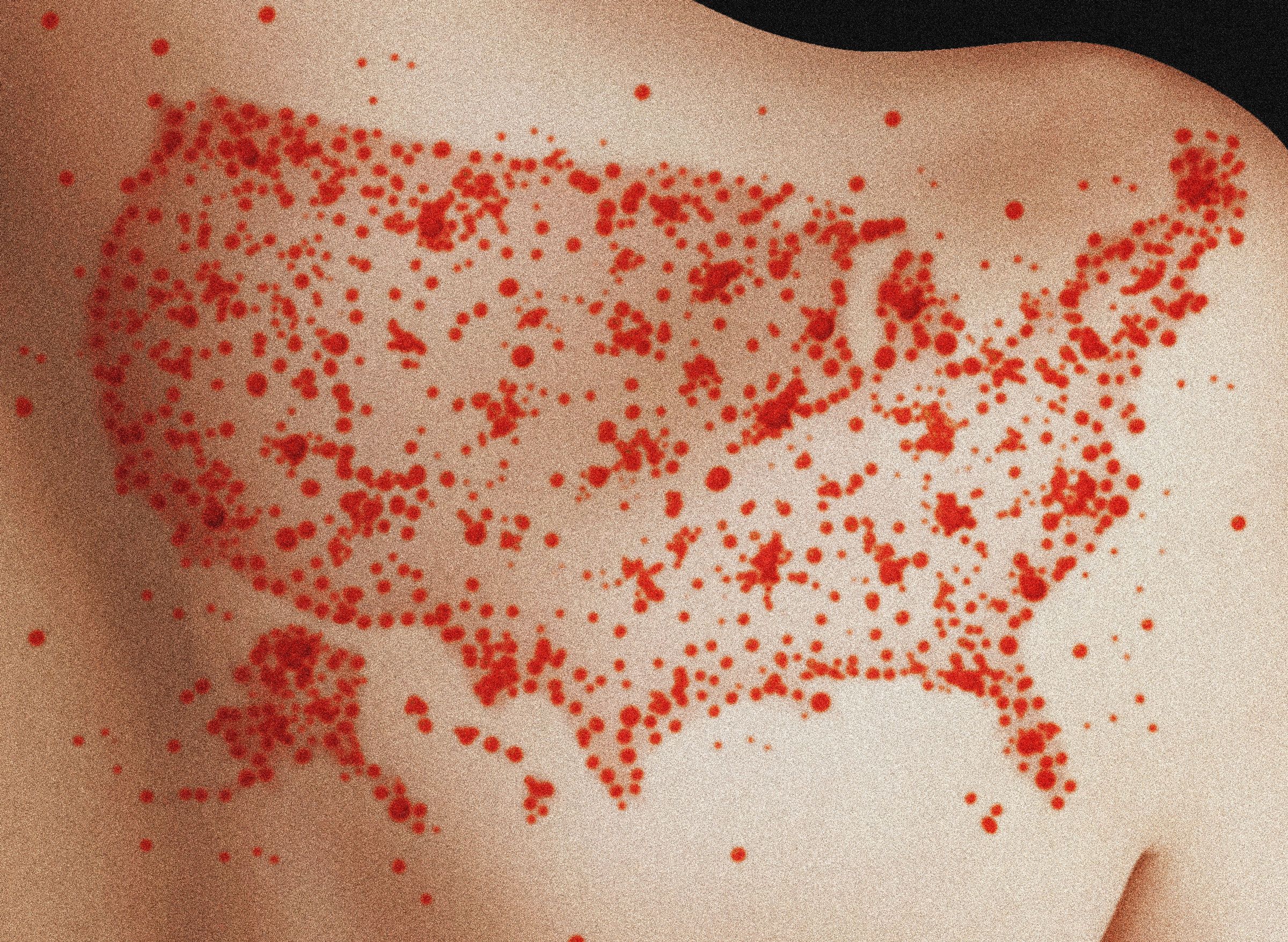
With vaccination rates among US kindergarteners steadily declining in recent years and Secretary of Health and Human Services Robert F. Kennedy Jr. vowing to reexamine the childhood vaccination schedule, measles and other previously eliminated infectious diseases could become more common. A new analysis published today by epidemiologists at Stanford University attempts to quantify those impacts.
Using a computer model, the authors found that with current state-level vaccination rates, measles could reestablish itself and become consistently present in the United States in the next two decades. Their model predicted this outcome in 83 percent of simulations. If current vaccination rates stay the same, the model estimated that the US could see more than 850,000 cases, 170,000 hospitalizations, and 2,500 deaths over the next 25 years. The results appear in the Journal of the American Medical Association.
“I don’t see this as speculative. It is a modeling exercise, but it’s based on good numbers,” says Jeffrey Griffiths, professor of public health and community medicine at Tufts University School of Medicine in Boston, who was not involved in the study. “The big point is that measles is very likely to become endemic quickly if we continue in this way.”
The United States declared measles eliminated in 2000 after decades of successful vaccination campaigns. Elimination means there has been no chain of disease transmission inside a country lasting longer than 12 months. The current measles outbreak in Texas, however, could put that status at risk. With more than 600 cases, 64 hospitalizations, and two deaths, it’s the largest outbreak the state has seen since 1992, when 990 cases were linked to a single outbreak. Nationally, the US has seen 800 cases of measles in 2025 so far, the most since 2019. Last year, there were 285 cases.
“We’re really at a point where we should be trying to increase vaccination as much as possible,” says Mathew Kiang, assistant professor of epidemiology and population health at Stanford University and one of the authors of the paper.
Childhood vaccination in the US has been on a downward trend. Data collected by the Centers for Disease Control and Prevention from state and local vaccination programs found that from the 2019–2020 school year to the 2022–2023 school year, coverage among kindergartners with state-required vaccinations declined from 95 percent to approximately 93 percent. Those vaccines included MMR (measles, mumps, and rubella), DTaP (diphtheria, tetanus, and acellular pertussis), polio, and chickenpox.
In the current study, Kiang and his colleagues modeled each state separately, taking into account their vaccination rates, which ranged from 88 percent to 96 percent for measles, 78 percent to 91 percent for diphtheria, and 90 percent to 97 percent for the polio vaccine. Other variables included demographics of the population, vaccine efficacy, risk of disease importation, typical duration of the infection, the time between exposure and being able to spread the disease, and the contagiousness of the disease, also known as the basic reproduction number. Measles is highly contagious, with one person on average being able to infect 12 to 18 people. The researchers used 12 as the basic reproduction number in their study.
Under a scenario with a 10 percent decline in measles vaccination, the model estimates 11.1 million cases of measles over the next 25 years, while a 5 percent increase in the vaccination rate would result in just 5,800 cases in that same time period.
In addition to measles, the authors used their model to assess the risk of rubella, polio, and diphtheria. The researchers chose these four diseases for their infectiousness and risk of severe complications. While sporadic cases of these diseases do occur and are usually related to international travel, they are no longer endemic in the US, meaning they no longer regularly occur.
The model predicted that rubella, polio, and diphtheria are unlikely to become endemic under current levels of vaccination. Rubella and polio have a basic reproduction number of four, while diphtheria’s is less than three. In 81 percent of simulations, vaccination rates would need to fall by around 35 percent for rubella to become endemic in the next 25 years. Polio, meanwhile, had a 50 percent chance of becoming endemic if vaccination rates dropped 40 percent. Diphtheria was the least likely disease to become reestablished.
“Any of these diseases, under the right conditions, could come back,” says coauthor Nathan Lo, a Stanford physician and assistant professor of infectious diseases.
To evaluate the validity of the model, the researchers ran a scenario with recent state-level vaccine coverage rates over a five-year period and found that the number of model-predicted cases broadly aligned with the number of observed cases in those years. The authors also found that Texas was at the highest risk for measles.
One limitation of the study was that the model assumed that vaccination rates were the same across all communities within a state. It didn’t take into account large variations in vaccination levels. Pockets of low vaccination rates, like in the Mennonite community at the center of the West Texas outbreak, would likely lead to local outbreaks that are larger than expected given the overall vaccination rate.
The study also didn’t take into account the possibility that vaccination rates could rebound in an area in response to an outbreak. “That’s the thing that we have control over. If you’re able to change that cycle, then that disease won’t spread anymore,” says Mujeeb Basit, associate chief of the Clinical Informatics Center at UT Southwestern Medical Center, who wasn’t involved in the study.
Kiang and Lo say the full impact of decreased vaccination will likely not be seen for decades. “It’s important to note that it’s totally feasible that vaccinations go down and nothing happens for a little while. That’s actually what the model says,” Kiang says. “But eventually, these things are going to catch up to us.”